This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
Diagnostic imaging
Breast Ultrasound
Sonomammography – i.e. breast ultrasound is a basic, non-invasive and painless examination, necessary in the correct diagnosis of breast lumps. Ultrasound examination is safe – it can be performed in pregnant women without affecting the condition of the fetus. There are also no obstacles or contraindications to perform an ultrasound while breastfeeding your baby.
Thanks to modern ultrasound devices, we can obtain a reliable image both in 2D and 3D (three-dimensional image).
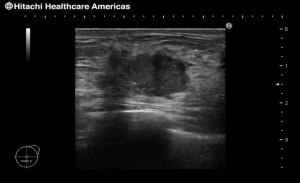
Breast ultrasound performed with the use of the highest-class apparatus allows to accurately determine the size of the lesion with an accuracy of 0.1 mm located in the mammary gland. Regular breast ultrasound (prophylactically every 6 months) – combined with self-examination and mammography (after 40 years of age) – is an essential element of breast cancer prevention, allowing for early detection and treatment of a lesion.
The latest generation equipment - uncompromising image quality in every detail
- – Super-precise image of the tumor with an accuracy of 0.1 mm – the most modern ultrasound heads made with Japanese perfection and using advanced technologies Multi-Layered, Single Cristal, Capacitive Micro-machined
- Real – Time 3D (4D) – 3D imaging in real time (so-called 4D)
- Elastography – Real-time Tissue Elastography (RTE) – real-time elastography and Shear Wawe Measurment (SWM) – provide with exceptional precision the assessment of the stiffness of the examined tumor tissues (the harder the more suspect)
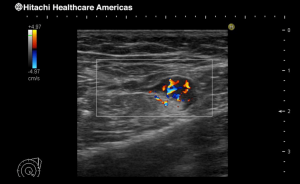
- Detective Flow Imaging – (DFI) while maintaining a very high Frame Rate (image smoothness) and the Doppler option of vascular flows in the examined tumor provides microflow imaging unattainable in other devices
- Contrast Harmonic Imaging CHI
- RVS fusion of ultrasound images with Magnetic Resonance Imaging (MRI) and Computed Tomography (CT) examinations, which allows for advanced biopsy planning
- Presentation of spacious and precise color photos, which are the basis for the diagnosis of breast tumors
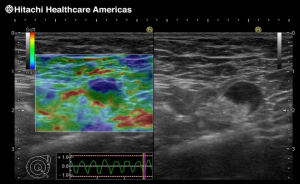
Breast elastography on Hitachi Arietta 750 ultrasound machines in the diagnosis of breast tumors
Elastography, i.e. determining the hardness of a nodule, is of great importance in distinguishing a benign nodule from breast cancer. Breast diagnostics is the most natural and the most common application of elastography, not only because of its superficial position, but also because of the close relationship between the malignancy of breast lesions and their hardness.
Breast elastography is crucial for the differentiation of benign (less hard) breast lumps from breast cancer (harder tumor), which is crucial for further management. Elastography is most often used to prove the benign nature of the lesion and to remove biopsy indications where it is not needed. It often provides additional information about seemingly mild changes.
At the patient’s request, we enable the transfer of examination documentation in digital form (any electronic carrier) – it is possible to conveniently recreate the diagnostic procedure.
Mammography
Mammography is an imaging test that uses a small dose of X-rays. Mammography involves taking two x-rays of both breasts. The obtained image in mammography allows to detect the so-called asymptomatic changes in the early stage, when they are not yet palpable or changes that are not visible on breast ultrasound, for example microcalcifications.
Mammography is not better or worse than breast ultrasound. Together with ultrasound, they complement each other. It should be remembered that we perform prophylactic mammography every 2 years after the age of 40.

Breast MRI
Magnetic Resonance Imaging (MRI) allows you to obtain anatomical images of the breast without the use of X-rays. This method, using a magnetic field and radio waves, is able to detect changes of about 2mm.
Breast MRI, has a very high diagnostic sensitivity of up to 97%. As a result, MRI enables early detection of asymptomatic changes, which are often not visible in a classic mammography examination.
emember that despite the significant technological development of equipment for breast imaging diagnostics,
it was not possible to create an apparatus that would give a 100% accurate diagnosis of the lesion.
A certain diagnosis can only be achieved by histopathological examination of the suspected nodule
(absolutely no pap smear after fine needle biopsy – FNAB).